Chapter 1: Introduction to Electronic Health Records
Learning Objectives:
- Define EHR and its core functions.
- Understand health IT interoperability.
- Explore EHR’s impact on patient care and health care providers.
- Discuss SHIN-NY’s benefits for New York’s Qualified Entities.
- Describe Meaningful Use and the Merit-based Incentive Payment System.
- Learn flat file and relational database principles.
An electronic health record (EHR) is a dynamic and patient-centered digital record system that provides instant and secure access to pertinent health information for authorized individuals in real-time. In the modern healthcare landscape, EHR systems have transformed how healthcare data are managed, providing seamless access to patient information in a user-friendly format. EHRs are digital versions of patients’ paper charts and are fundamental to modern healthcare operations.
The Digital Transformation in Healthcare
EHR systems have transformed healthcare delivery by facilitating improved patient care, increased patient participation, enhanced care coordination, and better diagnostics leading to improved patient outcomes. Moreover, EHR systems streamline practice efficiencies and generate cost savings. In today’s digital age, where technology is everywhere in our lives, EHR ensures a seamless flow of information within healthcare infrastructure, enabling access to vital information whenever and wherever it’s needed. This digital transformation in medicine underscores the importance of leveraging technology to optimize healthcare delivery and compensation.
Core Functions of EHRs
EHR systems offer a comprehensive solution to healthcare data management, extending beyond basic clinical information typically found in a provider’s office. Core functions of EHRs include capturing and storing health information such as medical histories, diagnoses, medications, treatment plans, immunization dates, allergies, radiology images, and laboratory and test results. They facilitate real-time, patient-centered records that make information available instantly and securely to authorized users. A significant advantage of EHRs is that they support other care-related activities directly or indirectly through various interfaces, including evidence-based decision support, quality management, and outcomes reporting (Office of the National Coordinator for Health Information Technology). Additionally, EHRs are designed to streamline the workflow in healthcare settings and enable comprehensive statistical reporting in compliance with health regulations.
The core functions of EHRs include several critical aspects:
Health Information and Data
EHRs collect clinical data regarding patients’ diagnoses, allergies, lab test results, and medications. This foundational function ensures a holistic view of a patient’s health history.
Result Management
EHRs streamline the organization and accessibility of test and lab results. Timely access to these critical data points aids in informed decision-making by healthcare providers.
Order Management
EHRs facilitate medical orders, including prescriptions, referrals, and diagnostic tests. By automating order management, EHRs enhance workflow efficiency and reduce errors.
Decision Support
EHRs offer evidence-based tools to guide clinical decisions. These tools improve care quality and patient outcomes by providing relevant information at the point of care.
Electronic Communication and Connectivity
EHRs enable secure data exchange among healthcare professionals. Seamless communication enhances collaboration and care coordination.
Patient Support
EHRs empower patients through health management tools like patient portals and self-monitoring apps. Patients can actively engage in their care by accessing their health information.
Administrative Processes and Reporting
EHRs simplify administrative tasks such as billing, scheduling, and documentation. Efficient administrative processes contribute to overall practice management.
Data Analysis and Reporting for Public Health
EHRs play a role in population health by collective and reporting data for public health initiatives. These functions aid in disease surveillance, quality improvement, and research.
In summary, EHRS are not only repositories of patient information but also powerful tools that enhance decision-making, streamline workflows, and ultimately contribute to better patient outcomes.
Discussion Questions
- How do EHR systems improve the quality of patient care compared to traditional paper records?
- In what ways do EHR systems help healthcare providers manage their daily tasks more efficiently?
Understanding Health IT Interoperability
Interoperability in healthcare refers to the ability of different healthcare information systems and software applications to communicate with each other, exchanging and utilizing information seamlessly. For systems to be interoperable, they generally need to use common data formats, allowing them to understand and process shared data.
In contrast to some countries like Japan, where EHR systems are interconnected through a unified chip system allowing any doctor to access a patient’s health information easily, the U.S. faces significant challenges. For example, major healthcare providers like Mount Sinai Health System and NYU Langone Health both utilize the Epic EHR system. While they operate independently, they have recently joined the nationwide interoperability framework through Epic’s Qualified Health Information Network (QHIN). This collaboration allows them to share patient health information more seamlessly, enhancing care coordination and improving overall efficiency. However, they are not directly interconnected. This lack of connectivity means that when patients visit different healthcare providers, their EHRs are not readily accessible across systems. Consequently, this can lead to redundancy in testing and gaps in efficiently sharing patient information. The U.S. healthcare system is characterized by the use of multiple vendors and lacks a standardized nationwide EHR system, complicating efforts towards achieving interoperability.
Advantages of Interoperability in Healthcare
Interoperability in healthcare provides several critical advantages that significantly enhance both individual patient care and broader healthcare operations.
Enhanced Patient Care
By facilitating seamless access to critical health information when and where it is needed, interoperability helps clinicians deliver safe, effective, and patient-centered care. This seamless data exchange supports informed decision-making, ultimately leading to improved patient outcomes.
Empowering Individuals and Caregivers
Interoperability also offers new ways for individuals and caregivers to engage with electronic health information. Through tools like patient portals, patients can take an active role in managing and coordinating their care, accessing pertinent health data that can influence their health decisions and actions.
Integral to Healthcare Activities
Interoperability has become an essential component of various healthcare activities, ranging from promoting health equity to enhancing the response capabilities during public health emergencies. Its role in integrating diverse health data sources is pivotal, strengthening efforts to improve outcomes across the healthcare spectrum.
The Vision for an Interoperable Health IT Ecosystem by 2024
The paper, “Connecting Health and Care for the Nation: A 10-Year Vision to Achieve an Interoperable Health IT Infrastructure,” outlines an ambitious roadmap for the next decade, aiming to revolutionize the U.S. healthcare system through enhanced interoperability. As we approach the 2024 milestone set in the vision, this paper remains highly relevant in reflecting ongoing challenges and goals in the U.S. healthcare IT landscape. It visualizes a robust interoperable health IT ecosystem where essential data is seamlessly accessible to the appropriate stakeholders, fostering a continuous learning health system. Such an infrastructure aims to lower healthcare costs, improve population health, empower consumers more significantly, and drive innovation by ensuring that all individuals, their families, and care providers can send, receive, find, and use health information effectively and securely. Figure 1 in the paper illustrates how various components of the healthcare system – providers, patients, payers, and researchers – are interconnected through a common framework that supports data exchange and real-time access to health information. This visual representation underscores the integrated approach required to achieve true interoperability, highlighting its potential to transform healthcare delivery by making it more coordinated, efficient, and patient-focused.
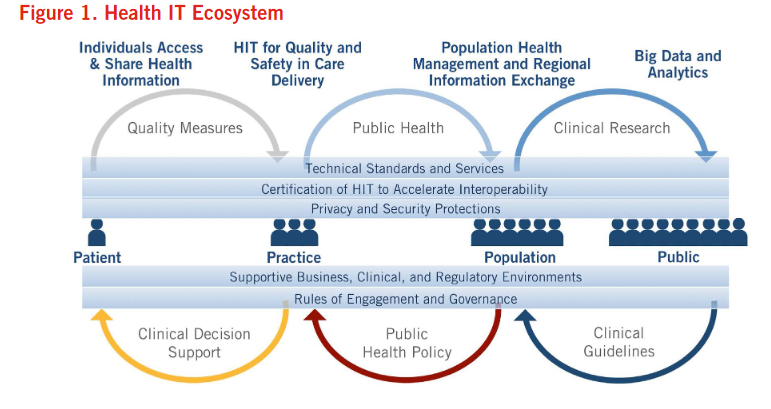
“Figure 1. Health IT Ecosystem” by The Office of the National Coordinator for Health Information Technology is in the Public Domain, CC0
Discussion Questions
- Why is interoperability important in healthcare, and how does it benefit patient care?
- What challenges does the U.S. face in achieving interoperability in its healthcare system, and what steps are being taken to address these issues?
Impact of EHRs on Care
Our rapidly evolving digital landscape, shaped by technologies like smartphones, tablets, and web-based devices, has revolutionized our daily lives and communication patterns. In the realm of medicine, where information is paramount, EHRs play a pivotal role.
Seamless Information Flow
A well-designed digital health care infrastructure, operated by EHRs, facilitates a seamless flow of information. This interconnected ecosystem leverages digital advancements to transform the delivery and compensation of care. Let’s explore the key impacts:
Improved Patient Care
EHRs empower clinicians with comprehensive patient data at their fingertips. Timely access to medical history, test results, and treatment plans enhances decision-making and patient outcomes.
Increased Patient Participation
Patients can actively engage in their health journey through EHR-based portals. Access to personal health records fosters informed decision-making and shared decision processes.
Enhanced Care Coordination
EHRs bridge gaps between care providers, enabling seamless transitions across settings. Coordinated care plans, medication reconciliation, and referrals lead to better continuity of care.
Improved Diagnostics & Patient Outcomes
EHRs facilitate data-driven diagnoses by aggregating clinical information. Real-time alerts and decision support tools aid in early detection and evidence-based interventions.
Practice Efficiencies and Cost Savings
Streamlined workflows, automated documentation, and billing efficiencies reduce administrative burden. EHRs contribute to cost-effective care delivery.
In summary, EHRs empower a data-rich health care landscape, where information flows effortlessly, benefiting patients, providers, and the entire health ecosystem.
Let’s explore a case study that highlights the impact of EHRs on Patient Outcomes:
Impact of Providing Patients Access to EHRs
A systematic review and meta-analysis assessed the effect of sharing EHRs with patients on various measures of quality of care. Here are the key findings:
Reduced HbA1c Levels
- Sharing EHRs with patients effectively reduces HbA1c levels.
- Improved glycemic control positively impacts patients with diabetes.
Positive Effects on Patient-Centeredness
- Overall, studies reported positive effects on patient-centeredness.
- Patients felt more engaged and informed about their health.
Health Outcomes and Preventative Services
- EHR access correlated with better health outcomes.
- Adherence to preventative services improved.
However, the authors emphasized the need for more robust studies to quantitatively assess the impact of sharing EHRs with patients.
This case study underscores how EHRs empower patients, enhance communication, and contribute to better health outcomes.
Discussion Questions
- How do EHRs improve patient care and outcomes for both patients and healthcare providers?
- In what ways do EHRs engage patients in their own healthcare, and why is this important for their overall health?
Government Role in EHR Implementation in New York State (NYS)
The New York State government has been a driving force in advancing health information technology (Health IT) infrastructure, particularly through the establishment of the Statewide Health Information Network for New York (SHIN-NY). This initiative aims to create an interconnected system that addresses critical challenges faced by New York’s health care system, including preventable medical errors, disparities in care quality, high costs, administrative inefficiencies, and lack of coordination among providers.
The SHIN-NY serves as the organizational infrastructure for this ambitious vision. Here are key aspects of its role:
Policy Framework and Governance
The SHIN-NY’s policy and governance framework provides the foundation for a comprehensive, interoperable health information infrastructure. It ensures that data flows securely and efficiently across the health care ecosystem.
Collaborative Processes and Accountability
The SHIN-NY involves collaboration among various stakeholders, including the New York State Department of Health (NYS DOH), the New York eHealth Collaborative (NYeC), and Qualified Entities (QEs). NYS DOH oversees and enforces SHIN-NY regulations, sets strategy, and approves policy and investment. NYeC leads, coordinates, and administers the SHIN-NY, advising NYS DOH on policy development. The QEs manage technical connections with data contributors, implement SHIN-NY policies and deliver local services.
Qualified Entities (QEs)
Six QEs serve all of New York: Bronx RHIO, Healtheconnections, Healthelink, Healthix, HIXNY, and Rochester RHIO (Figure 2). These QEs facilitate secure electronic connections with participating health care providers, allowing data to flow seamlessly. QE participants include hospitals, clinics, nursing homes, Federally Qualified Health Centers (FQHCs), home care agencies, payers, ambulatory practices, Emergency Medical Services (EMS) agencies, pharmacies, and community-based organizations (CBOs).
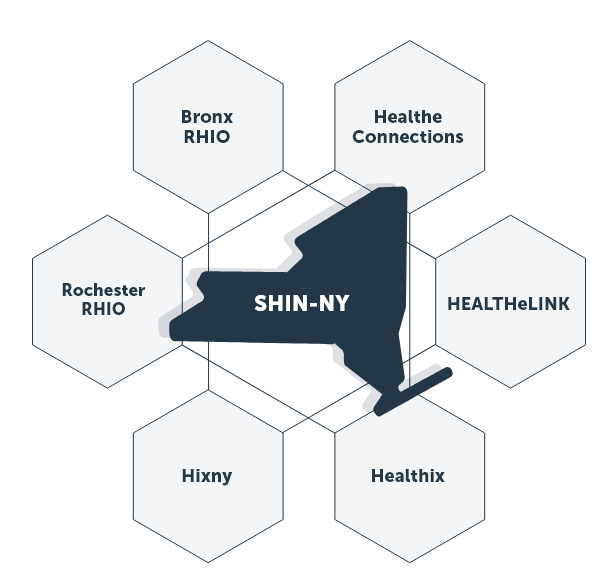 “Figure 2: New York’s Interconnected Qualified Entities” by New York eHealth Collaborative (NYeC) is in the Public Domain, CC0
“Figure 2: New York’s Interconnected Qualified Entities” by New York eHealth Collaborative (NYeC) is in the Public Domain, CC0
Impact on Patient Care
With patient consent, participating providers access the SHIN-NY to improve care delivery. EHRs play a pivotal role in this ecosystem, enabling timely access to critical patient information.
In summary, the government’s commitment to the SHIN-NY underscores its dedication to creating an interoperable health IT landscape that benefits patients, providers, and the entire health care community.
Key Facts about the SHIN-NY
The SHIN-NY connects 100% of the hospitals in New York State, over 100,000 healthcare professionals, and represents millions of people living in or receiving care in New York.
Core services provided by QEs include:
- Statewide Patient Record Lookup (sPRL): Access to comprehensive patient information.
- Notifications/Alerts: Timely updates on patient events.
- Secure Direct Messaging: Secure communication among providers.
- Lab results delivery (Upstate only).
- Provider and Public Health Clinical Viewers: Enhanced visibility into patient data.
- Consent Management: Managing patient consent preferences.
Impact of SHIN-NY Usage
Use of the SHIN-NY is associated with:
- 50% reduction in the rate of hospital readmissions.
- 26% reduction in the rate of emergency department visits.
- 35% reduction in the rate of repeat imaging procedures.
Watch this informative Video 1 about the SHIN-NY to learn more:
“Video 1: The Statewide Health Information Network for New York (The SHIN-NY)” by NYeHealth is in the Public Domain, CC0
Discussion Questions
- How does the Statewide Health Information Network for New York (SHIN-NY) improve the coordination and quality of patient care?
- What are some specific benefits and challenges of implementing an interconnected health information network like SHIN-NY in New York State?
Meaningful Use and the Shift to the Merit-Based Incentive Payment System (MIPS)
Meaningful Use (MU), once a cornerstone of healthcare transformation, underwent a significant evolution with the advent of the Medicare Access and CHIP Reauthorization Act (MACRA). Let’s delve into the background and rationale behind this transition:
Background: Medicare EHR Incentive Program (Meaningful Use)
The Medicare EHR Incentive Program, commonly known as meaningful use, aimed to encourage healthcare providers to adopt and effectively use certified EHR technology. It emphasized data capture, interoperability, and patient engagement. However, as healthcare evolved, so did the need for a more comprehensive approach.
MACRA and the Birth of MIPS: A Paradigm Shift
In 2015, MACRA was enacted, signaling a bipartisan effort to reform Medicare payments. MACRA introduced the Quality Payment Program (QPP), which replaced the sustainable growth rate formula. With QPP, the MIPS emerged as a transformative force. MIPS consolidated multiple quality programs, including meaningful use, the Physician Quality Reporting System (PQRS), and Value-Based Payment Modifiers (VBPM). The goal was to streamline reporting, enhance quality, and align incentives.
MIPS Components: Harmonizing Quality Programs (Figure 3)
Quality (Replaces PQRS):
- Accounts for 60% of the MIPS Final Score.
- Focuses on clinical quality measures and outcomes.
Cost (Resource Use):
- Not counted in 2017, but gradually becomes 30% of the Final Score by 2019.
- Analyzes claims data to assess the cost of patient care.
Promoting Interoperability (PI, Replaces MU):
- Encourages the use of certified EHR technology.
- Facilitates secure health information exchange.
Improvement Activities (New Component):
- Accounts for 15% of the Final Score.
- Rewards practices that prioritize improvement efforts (e.g., care coordination, patient safety).
In summary, MIPS represents a unified approach, fostering quality care, reducing administrative burden, and aligning incentives for healthcare providers.
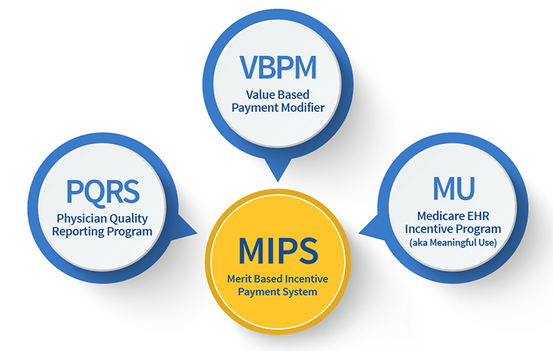 “Figure 3: Meaningful Use and the Shift to the Merit-based Incentive Payment System” by HealthIT.gov is in the Public Domain, CC0
“Figure 3: Meaningful Use and the Shift to the Merit-based Incentive Payment System” by HealthIT.gov is in the Public Domain, CC0
The Transition from MU to Advancing Care Information (ACI)
MU leveraged certified EHR technology for various purposes. However, as healthcare policies evolved, the ACI category within the MIPS took its place. Despite this shift, the core objectives remain consistent:
Improve Quality, Safety, and Efficiency
ACI continues to focus on enhancing care quality, reducing errors, and streamlining processes. EHRs play a pivotal role in achieving these goals.
Engage Patients and Family
ACI encourages active patient participation through EHR-based portals. Access to health information empowers patients in their care decisions.
Enhance Care Coordination
Seamless data exchange remains critical for better care coordination. Providers can access vital patient information when needed.
Population and Public Health
ACI contributes to population health management. EHRs facilitate data-driven public health initiatives.
Privacy and Security
Safeguarding patient privacy and maintaining health information security remains paramount. EHRs adhere to strict security protocols.
Discussion Questions
- How does the transition from Meaningful Use (MU) to the Merit-based Incentive Payment System (MIPS) streamline reporting and incentivize quality care for healthcare providers?
- What are the key components of MIPS, and how do they contribute to improving healthcare quality and outcomes?
Database Systems in EHRs: Comparing Flat File and Relational Databases
Flat file databases and relational databases represent two fundamentally different approaches to data management, each with implications for their use in EHR systems. Flat file databases store all data in a single table format with no relationships between tables, a method developed by IBM in the early 1970s. Due to their simplicity, flat file systems are easy to implement and manage but lack efficiency and robust security measures, which are crucial for handling sensitive health information.
On the other hand, relational databases are structured to organize data across multiple tables interconnected by keys, enhancing data integrity and security. This model supports complex querying and data manipulation, making it ideal for the multifaceted needs of modern EHR systems, which require the handling of large datasets and simultaneous access by multiple users. The ability of relational databases to ensure accurate, secure, and efficient data management aligns well with the critical requirements of EHRs, which aim to store comprehensive, interconnected patient health records securely and efficiently.

“Figure 4: Flat File vs Relational Database” by DatabaseTown.com is in the Public Domain
Here’s a comparison table highlighting the key differences between flat file and relational databases:
|
Feature |
Flat File Database |
Relational Database |
|
Structure |
Single table |
Multiple related tables |
|
Data Integrity |
No built-in mechanism |
Enforced via primary/foreign keys |
|
Data Model |
Flat data model |
Relational data model |
|
Data Access |
Simple file input/output (I/O) operations |
Complex queries with Structured Query Language (SQL) |
|
Performance |
Can be slow with large datasets |
Optimized with indexes and caching |
|
Scalability |
Not suited for large data or concurrent access |
Handles large data and multiple users |
Discussion Questions
- What are the advantages and limitations of flat file databases compared to relational databases in the context of managing electronic health records (EHRs)?
- How do relational databases address the challenges faced by flat file databases in handling large datasets and ensuring data integrity and security in EHR systems?
Key Terms
Care Coordination: The integration of services across healthcare providers facilitated by EHRs.
Decision Support: Real-time, evidence-based guidance by EHRs to healthcare professionals.
Data Exchange: The seamless sharing of health information among healthcare systems.
Interoperability Framework: The structured approach that enables diverse health IT systems to communicate effectively.
Care Continuity: Ensuring uninterrupted and consistent patient care across different healthcare settings via EHRs.
Patient Empowerment: Enabling patients to actively participate in their healthcare decisions through access to EHRs.
SHIN-NY Governance: Oversight and policy direction for New York’s Statewide Health Information Network.
Qualified Entities (QEs): Organizations facilitating data exchange among healthcare providers in New York.
Meaningful Use (MU): A program aimed at promoting the adoption of certified EHR technology to improve healthcare quality and efficiency.
Merit-Based Incentive Payment System (MIPS): A system under Medicare Access and CHIP Reauthorization Act (MACRA) that consolidates various quality reporting programs to streamline reporting and improve healthcare outcomes.
Flat File Databases: A simple database system that stores all data in a single table without relationships, typically easier to manage but less efficient and secure.
Relational Databases: A database system that organizes data into multiple tables linked by keys, offering enhanced security, data integrity, and support for complex queries.
Exercises
Exercise 1: True or False
Instructions: Read the statements below and indicate whether they are True or False.
EHRs only store patient information but do not assist in any decision-making processes.
Interoperability in healthcare leads to improved care coordination and seamless communication among healthcare providers.
The SHIN-NY is mainly focused on ensuring that healthcare providers in New York compete rather than collaborate.
Meaningful Use was completely discarded and has no influence on current EHR practices.
Exercise 2: Fill in the Blanks
Instructions: Complete the sentences with the correct terms from the provided options.
EHRs improve healthcare administration by streamlining tasks such as _______, scheduling, and documentation. Options: billing, staffing, purchasing
SHIN-NY contributes to public health by providing _______, which help manage disease outbreaks and health monitoring. Options: statewide patient record lookups, private health consultations, individual treatment plans
The transition from Meaningful Use to _______ marked a shift in focus towards integrated care and quality improvement under MACRA. Options: MIPS, ACI, CDC
Exercise 3: Multiple Choice Questions
Instructions: Choose the correct answer for each question.
What is a core function of EHRs concerning patient data?
A) Data deletion
B) Data analysis
C) Data storage
D) All of the above
How does interoperability benefit patients directly?
A) By decreasing their involvement in care decisions
B) Through increased healthcare costs
C) By providing access to health data through patient portals
D) By limiting information flow to doctors only
Exercise 4: Short Answer
Instructions: Provide a short answer to the following questions.
Describe one way in which EHRs enhance patient care.
What role does the New York eHealth Collaborative (NYeC) play in the SHIN-NY?
Exercise 5: Scenario Analysis
Instructions: Read the scenario and answer the question that follows.
Scenario: A patient visits three different healthcare facilities in a month due to a chronic condition. Each facility uses a different EHR system, and there is no interoperability between these systems.
Question: What challenges might arise from this situation, and how could interoperability address these challenges?
Lab Exercise 1: Designing a Simple Database
Objective: To understand the practical differences between flat file and relational database systems by designing and implementing a simple database for a small clinic’s EHR.
Materials Needed:
Computer with access to database software (e.g., Microsoft Access for a flat file database and MySQL for a relational database).
Sample patient data to populate the database.
Instructions:
Design Phase:
Create a design for a flat file database using Microsoft Access. The database should include one table with fields such as PatientID, Name, Age, Allergies, Diagnoses, and VisitDate.
Create a design for a relational database using MySQL. The database should include multiple tables:
Patients (PatientID, Name, Age)
Visits (VisitID, PatientID, VisitDate, DoctorID)
Medical Conditions (ConditionID, PatientID, Diagnosis, Allergy)
Doctors (DoctorID, Name, Specialty)
Draw entity-relationship diagrams for both databases.
Implementation Phase:
Implement both database designs:
Use Microsoft Access to create the flat file database and populate it with sample data.
Use MySQL to create the relational database schema and populate it with the same sample data.
Ensure that in the relational database, relationships are enforced with primary and foreign keys.
Testing and Querying:
Perform basic data entry tasks on both databases.
Query both databases to retrieve a list of patients who visited on a specific date.
Analyze the performance and ease of use of each system when performing the query.
Analysis:
Write a brief report comparing the two types of databases in terms of setup complexity, data integrity, querying capability, performance, and scalability.
Discuss which database model would be more suitable for a large hospital’s EHR system and why.
Deliverables:
Entity-relationship diagrams for both databases.
Screenshots of both implemented databases with sample data.
A written report on the findings and recommendations.
Lab Exercise 2: Data Integrity and Security in Database Systems
Objective: To explore how data integrity and security are managed in flat file and relational databases, particularly in the context of EHRs.
Materials Needed:
Computer with database software (Microsoft Access and MySQL).
Sample scripts or commands to manipulate database data.
Instructions:
Preparation:
Use the databases created in Lab Exercise 1.
Prepare sample scripts to insert, update, and delete data in both databases.
Experimentation:
Flat File Database:
Execute scripts that attempt to insert duplicate data, delete data, and perform updates that could potentially violate data integrity (e.g., changing a PatientID).
Relational Database:
Execute similar scripts but observe how the database handles these operations with constraints like primary and foreign keys.
Security Testing:
Simulate basic security scenarios in both databases:
Attempt to access the database without proper authentication (if possible within the setup).
Try to execute SQL injections (in the case of the relational database).
Analysis:
Document how each database responds to the integrity and security tests.
Discuss the results in terms of the robustness of data integrity and security features in flat file vs. relational databases.
Deliverables:
A detailed log of all tests performed and their outcomes.
Screenshots documenting the test processes and results.
A comprehensive report discussing the importance of data integrity and security in EHRs and how these aspects are supported or compromised by each database type.
These exercises aim to give students practical experience with the key differences between database types, focusing on real-world applications in healthcare settings.
References
Office of the National Coordinator for Health Information Technology. (n.d.). What are the advantages of electronic health records? HealthIT.gov. Retrieved April 15, 2024, from https://www.healthit.gov/faq/what-are-advantages-electronic-health-records
Green, J. (January, 2023). EHR in Practice. What are the core functions of EHR? Retrieved April 15, 2024, from https://www.ehrinpractice.com/ehr-core-functions.html
Office of the National Coordinator for Health Information Technology. (n.d.). Interoperability. HealthIT.gov. Retrieved April 15, 2024, from https://www.healthit.gov/topic/interoperability
Office of the National Coordinator for Health Information Technology. (n.d.). Connecting Health and Care for the Nation: A 10-Year Vision to Achieve an Interoperable Health IT Infrastructure. Retrieved April 15, 2024, from https://www.healthit.gov/sites/default/files/ONC10yearInteroperabilityConceptPaper.pdf
Office of the National Coordinator for Health Information Technology. (n.d.). Impact of EHRs on Care. HealthIT.gov. Retrieved April 15, 2024, from https://www.healthit.gov/topic/health-it-and-health-information-exchange-basics/benefits-ehrs
Neves, A. L., Freise, L., Laranjo, L., et al. (2020). Impact of providing patients access to electronic health records on quality and safety of care: A systematic review and meta-analysis. BMJ Quality & Safety, 29(12), 1019-1032. https://psnet.ahrq.gov/issue/impact-providing-patients-access-electronic-health-records-quality-and-safety-care-systematic
New York State Department of Health. (n.d.). SHIN-NY Organizational Infrastructure. Health.NY.gov. Retrieved April 15, 2024, from https://www.health.ny.gov/technology/infrastructure/
New York eHealth Collaborative. (n.d.). What is the SHIN-NY? NYeHealth.org. Retrieved April 15, 2024, from https://www.nyehealth.org/shin-ny/what-is-the-shin-ny/
New York State Department of Health. (n.d.). Statewide Health Information Network for New York (SHIN-NY). Regs.Health.NY.gov. Retrieved April 15, 2024, from https://regs.health.ny.gov/sites/default/files/proposed-regulations/Statewide%20Health%20Information%20Network%20for%20New%20York%20%28SHIN-NY%29.pdf
New York eHealth Collaborative. (n.d.). The Statewide Health Information Network for New York (The SHIN-NY) [Video]. YouTube. https://youtu.be/O0nMDlv8CSg?si=mDtEHWrCX5mGKAos
American Medical Association. (2023, September 18). Understanding Medicare’s Merit-based Incentive Payment System (MIPS). https://www.ama-assn.org/practice-management/payment-delivery-models/understanding-medicare-s-merit-based-incentive-payment
HealthIT.gov. (n.d.). Meaningful use. Retrieved April 15, 2024, from https://www.healthit.gov/topic/meaningful-use-and-macra/meaningful-use
Centers for Medicare & Medicaid Services. (2023, September 6). MACRA: What’s MACRA? CMS.gov. Retrieved April 15, 2024, from https://www.cms.gov/medicare/quality/value-based-programs/chip-reauthorization-act
GeeksforGeeks. (2024, March 11). Flat file database. Retrieved from https://www.geeksforgeeks.org/flat-file-database/?ref=gcse
DatabaseTown. (n.d.). Relational Database vs Flat File (Differences & Similarities). Retrieved from https://databasetown.com/relational-database-vs-flat-file-differences-similarities/
